Breast cancer risk from HRT higher than thought, research shows
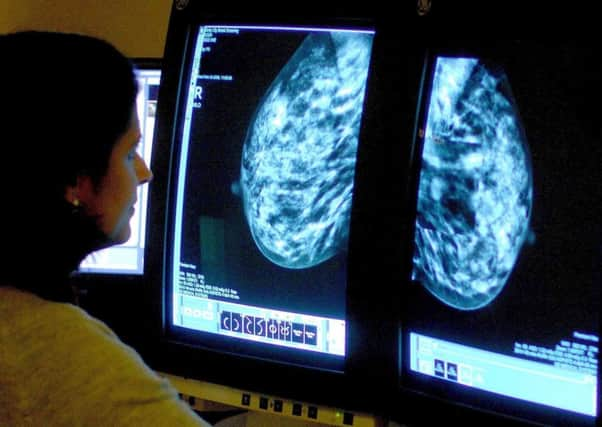

Taking the treatment to combat the effects of the menopause could mean that women are 2.7 times more likely to develop breast cancer than those who are not, a new study found.
Women taking combined HRT are more likely to develop the disease, with risk increasing the longer it is used, the study found.
Advertisement
Hide AdAdvertisement
Hide AdThe new study, published in the British Journal of Cancer, found that those taking oestrogen plus progestogen HRT were 2.74 times more likely to develop breast cancer.
And those who had been using the combined HRT for 15 or more years had a 3.27 times increased risk, the study found.
But once HRT-use ended the increased risk returned to normal levels, the authors stressed.
Those taking oestrogen-only HRT did not have an increased risk, they found.
Advertisement
Hide AdAdvertisement
Hide AdThe findings were drawn from thousands of women taking part in the Breast Cancer Now Generations Study - a major study following more than 100,000 women for 40 years to investigate the causes of breast cancer.
Experts analysed data over six years from almost 40,000 menopausal women - 775 of whom developed breast cancer.
HRT is used to treat symptoms of the menopause - such as hot flushes, migraines, disrupted sleep, mood changes and depression - by replacing hormones lost through the menopause.
For around 10% of women, symptoms can last for up to 12 years. The average age for menopause in the UK is 51.
Around one in ten women use HRT during their 50s.
Advertisement
Hide AdAdvertisement
Hide AdResearch has shown that HRT increases the risk of breast and ovarian cancer, while links have also been made with stroke and heart attack.
But the authors of the latest study said that previous studies could have underestimated the risk of breast cancer because they did not use updated information on women’s use of HRT over time and took into account when they actually began the menopause.
Earlier investigations may have underestimated the increased risk of breast cancer by up to 60%, the authors added.
“Our research shows that some previous studies are likely to have underestimated the risk of breast cancer with combined oestrogen-progestogen HRT,” said study lead author Anthony Swerdlow, professor of epidemiology at The Institute of Cancer Research, London.
Advertisement
Hide AdAdvertisement
Hide Ad“We found that current use of combined HRT increases the risk of breast cancer by up to threefold, depending on how long HRT has been used.
“Our findings provide further information to allow women to make informed decisions about the potential risks and benefits of HRT use.”
Baroness Delyth Morgan, chief executive at Breast Cancer Now, added: “Whether to use HRT is an entirely personal choice, which is why it’s so important that women fully understand the risks and benefits and discuss them with their GP. We hope these findings will help anyone considering the treatment to make an even more informed decision.
“On balance, some women will feel HRT to be a necessity. But in order to minimise the risk of breast cancer during treatment, it is recommended that the lowest effective dose is used for the shortest possible time.
Advertisement
Hide AdAdvertisement
Hide Ad“The good news is that the increased risk of breast cancer begins to fall once you stop using HRT.”
Meanwhile, a separate study has found that women who expect the worst from a type of breast cancer treatment are more likely to suffer adverse side-effects.
The research, published in the Annals of Oncology, found that women with a negative perception of receiving hormone therapies such as tamoxifen suffered nearly twice the number of side-effects than did women with positive expectations or who thought the effects would not be too bad.
The authors looked at 111 women in Germany who had treatment for hormone receptor positive breast cancer.
Advertisement
Hide AdAdvertisement
Hide AdThey questioned the patients about their expectations of the effect of taking adjuvant hormone therapy at the start of the trial and then assessed them at three months and at two years.
Those with higher expectations of side-effects at the start of the study saw a 1.8 increase in their occurrence after two years.
Professor Yvonne Nestoriuc, from the University Medical Centre, Hamburg, Germany, who led the study, said: “Our results show that expectations constitute a clinically relevant factor that influences the long-term outcome of hormone therapy.
“Expectations can be modified so as to decrease the burden of long-term side-effects and optimise adherence to preventive anti-cancer treatments in breast cancer survivors.”
Advertisement
Hide AdAdvertisement
Hide AdCommenting on the HRT study, Dr Heather Currie, spokeswoman for the Royal College of Obstetricians and Gynaecologists (RCOG) and chairwoman of the British Menopause Society (BMS), said HRT was an effective treatment.
She added: “However, the risks and benefits are different for each woman, depending on her own medical history, her family history and her menopausal symptoms. To take or not to take HRT, or other treatments for menopausal symptoms, is an individual choice.”